Our Services
Our Main Services
We offer integrated services combining healthcare, environmental experiences, accessibility, and professional training—ensuring a complete journey tailored to every client’s needs.

Medical tourism:
We provide access to top hospitals and expert doctors across Egypt, managing your entire treatment journey from medical consultation to recovery with the highest standards of care.

Environmental Tourism:
Our programs focus on natural healing experiences in Egypt’s eco-friendly destinations, offering clean environments and therapeutic landscapes that support recovery and well-being.

Accessible health tourism:
We deliver specialized services for elderly patients and people with disabilities, ensuring comfort, safety, and full accessibility throughout their medical and travel journey.

Training Tourism:
We offer medical training programs, workshops, and educational experiences in collaboration with leading healthcare institutions in Egypt.
Medical tourism:
Medical tourism in Egypt is supported by advanced hospitals, modern technology, and highly qualified doctors across multiple specialties. Egypt is known for its excellence in fertility treatments, cancer care, heart surgeries, eye treatments, and orthopedic procedures, all with high success rates.
Both the public and private sectors contribute to delivering high-quality healthcare, while continuous medical education attracts doctors from across the region for training and expertise.

Here is a short, professional English version suitable for a website:
Egypt Medical & Tourism Program
As part of our commitment to your health, we proudly present the Egypt Medical & Tourism Program, designed to provide the highest standards of healthcare through Noor Al Fouad Medical Complex, along with a network of specialized hospitals, medical centers, and expert consultants across all fields.
We take pride in being pioneers in delivering integrated services for Arab and international patients traveling to Egypt for treatment. From arrival to departure, we ensure a seamless experience by assisting with visa procedures, travel arrangements, accommodation, and transportation—while overcoming language and cultural barriers.
Our goal is to transform your medical journey into a comfortable and relaxing experience.
Our Services Include:
Airport Customer reception
Hotel bookings or furnished apartments
Professional translators (if needed)
Multilingual nursing staff
Medical report translation
Rehabilitation and physiotherapy services
Personalized dietary plans
Leisure and tourism programs
Medical check-ups for companions
Why Choose Us?
Our care continues even after you return home, with ongoing follow-up and remote medical support to ensure your full recovery.
Our Promise
We handle everything—from reviewing your medical case to arranging your full journey—so you can focus on healing, while enjoying your stay in Egypt.
Medical tourism relies on specialized hospitals, clinics, and medical centers equipped with advanced technology and highly qualified healthcare professionals.
Egypt is home to a large number of expert doctors across various medical specialties, making it a trusted destination for medical tourism. Both the public and private sectors play a key role in delivering high-quality healthcare services.
Egypt’s medical services are well known for their excellence, with leading doctors in different fields. There are many specialized centers for infertility and fertility treatments, achieving high success rates.
In addition, Egypt is highly recognized for treating various types of cancer, heart diseases, and performing advanced surgical procedures, positioning it as one of the leading countries in the region in these specialties. The same applies to ophthalmology, with many specialized eye hospitals using advanced technologies such as laser treatments. Egypt also achieves high success rates in treating hepatitis C, as well as joint diseases and orthopedic surgeries, including spine and limb procedures. Minimally invasive (endoscopic) surgeries are also available in advanced hospitals, along with many other distinguished specialties.
Moreover, the integration of both public and private sectors, along with continuous medical education in Egypt, attracts many doctors from Arab countries who come for training and study.
Comprehensive Solutions Covering Every Detail of Your Medical Journey
From treatment to travel, we provide fully integrated solutions covering all aspects of your medical journey. Even leisure activities and tours within Egypt are arranged through specialized companies in tourism and shopping.
TraveCare Egypt offers complete programs that include medical expenses, travel, accommodation, and local transportation, as well as recovery and wellness programs—tailored to each patient’s personal preferences and medical condition.
Our Specialized Team
TraveCare Egypt brings together a highly qualified team across all fields required to support the patient’s journey. This includes doctors, technicians, and nursing staff, along with medical service management experts.
Our team also includes financial consultants, personal care specialists, physiotherapists, rehabilitation experts, and nutritionists—ensuring comprehensive care at every stage.
We strive to deliver the highest standards of medical excellence in Egypt.
We ensure full protection of patients’ rights, providing complete transparency in diagnosis and treatment plans, along with detailed explanations for every stage of care.
TraveCare Egypt is committed to applying the highest international medical standards established by leading global healthcare institutions, ensuring top-quality treatment in Egypt.
We also maintain continuous medical follow-up throughout all stages of treatment, providing you with complete confidence and reassurance.
Your health is at the center of everything we do.
Environmental Tourism
Experience the natural power of Egypt’s climate, deserts, and mineral springs that promote physical and mental well-being — where nature itself becomes part of your healing journey.

Step 1:
Warm mineral-rich mud is applied to the body to draw out toxins and soothe inflammation.

Step 2:
The mud’s minerals absorb impurities and stimulate blood flow for deep healing.
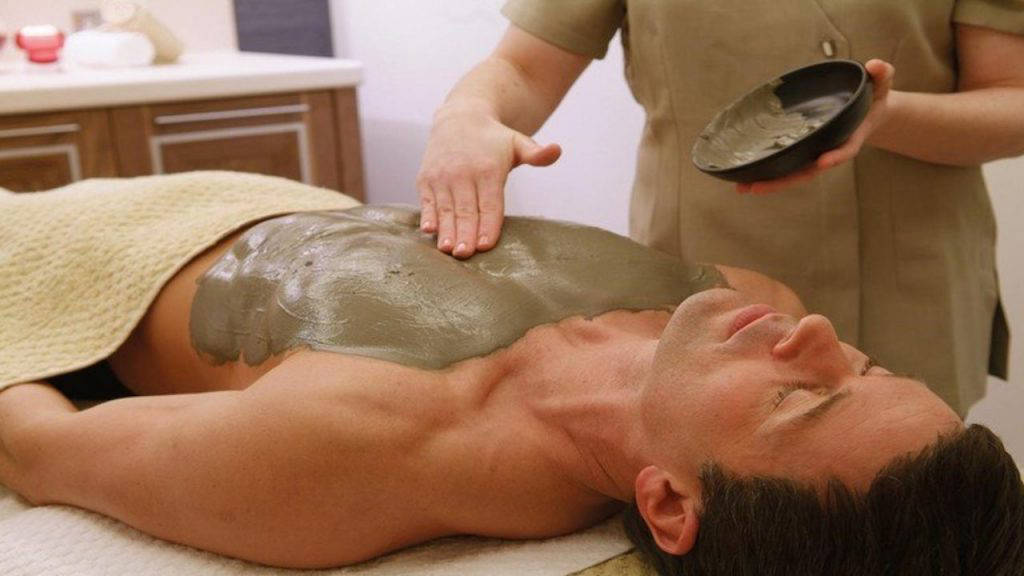
Step 3:
After cleansing, patients feel refreshed, with smoother skin, improved mobility, and lasting relaxation.

Step 1:
Patients bathe in natural sulfur springs rich in healing minerals that nourish the skin and body.

Step 2:
The minerals penetrate deeply, improving joint flexibility, skin health, and respiratory function.

Step 3:
The session ends with rest and hydration, leaving the body detoxified and revitalized.

Step 1:
The body is gently covered with warm desert sand, allowing natural heat to penetrate the muscles and joints.

Step 2:
The therapy stimulates blood circulation and releases toxins through sweating and heat absorption.

step 3:
After the session, patients rest and hydrate, experiencing pain relief, muscle relaxation, and renewed energy.
Environmental Healing Maps
Explore a curated network of natural healing destinations through our Environmental Healing Maps. From tranquil coastlines to therapeutic desert landscapes, we connect you with the best eco-healing spots across Travecare’s branches, designed to enhance recovery, relaxation, and overall well-being.
Our Services
or patients with damaged knee joints who require subsequent replacement of the natural joint, this surgeon uses a prosthetic knee joint procedure. In this procedure, an artificial knee joint is attached to the femur and the upper part of the bone is connected. A polyethylene sleeve is placed between the femur and the tibia to provide support. In approximately 50% of cases, the patella is also replaced. Read more in: Knee Joint
The main reason for knee replacement surgery is osteoarthritis of the knee, where the cartilage becomes unable to absorb shocks. There are many factors that contribute to knee osteoarthritis, such as weight loss, organ transplants, autoimmune deficiencies, rheumatoid arthritis, fractures, and some congenital factors. There are also several factors that affect the bones. Read more: Information about Knee Pain and Its Causes
Emerging Symptoms (Clinical Presentations)
Preoperative Complaints (Pre-Surgery Complaints)
Wearing, age, bowing of the knee, and previous injuries are all factors that contribute to erosion and changes in the knee joint.
(Pain)
Most people suffer from osteoarthritis of the knee, and the pain is usually felt in the knee joint. However, patients can often experience pain in the inner or outer chest, or behind the kneecap. Initially, the pain lasts for a prolonged period, known as “onset pain,” and then begins to subside after a few minutes. However, as the osteoarthritis progresses, the pain can occur in cold weather and may disrupt sleep at night.
Related Topics
Personal Symptoms
Knee Pain After Pilates Training
What are the Causes of Cartilage Degeneration in Bones?
To Treat the Disease Due to Cartilage Atrophy
What are the Alternative Surgical Options to Neck Arthroscopy for Osteoarthritis?
Stiffness and Rigidity in Progression (Stiffness/Rigidity)
This initially occurs during the night and morning, then gradually worsens, making it difficult for the patient to change clothes, shoes, and footwear, and also affecting their other daily activities.
Walking Difficulties (Waking Difficulties)
When knee erosion reaches an advanced stage, the patient will experience significant walking difficulties and pain. After some time, the patient may require assistive devices such as crutches. In most cases, cycling will be easier than walking.
Diagnosis
The treating physician must conduct preoperative examinations to accurately assess the patient’s condition. This includes asking about medication history and symptoms, examining the knee and then the other knee, and performing X-rays and MRI scans.
Medical Care
This surgical procedure aims to achieve pain-free mobility and restore full and permanent function, allowing for a full range of motion in all directions.
Knee replacement surgery is performed when there is an urgent need, such as in cases of severe mobility issues. The procedure, which takes between 60 and 90 minutes, involves placing three components of the knee joint. Part of the bone is comfortable, part of the muscles are comfortable, and part of the rest is sometimes provided by polyethylene.
The first day begins with a specific morning routine. After the second day, the medical team begins to move the knee, and after the fourth day, exercises begin in the hospital. Following this, the patient’s natural building blocks are prepared in their home environment, allowing them to gain experience in training those with limited mobility and performing stretching exercises for a full range of motion.
Physical Therapy and Rehabilitation
Pre-operative (Prior to surgery)
Rami teaches the patient some practical steps to ensure they are ready to perform these activities correctly after the operation. This facilitates a faster recovery. It is also important that the patient’s functional status is as good as possible before the surgery, which ensures a quick return to normal activity afterward. Read about the procedure: Knee Arthroscopy
Post-operative (Post-surgery)
Many studies examining the natural effects of treatment after knee replacement surgery consider physical therapy to be highly beneficial, such as sports therapy, balance exercises, or cycling. There are four new steps in joint reconstruction. The first step is to develop static strength, followed by dynamic strength (which is developed during movement), and finally, joint stabilization.
On the first day after surgery, activation begins with a crucial focus on improving blood circulation. On the second day, walking can begin using assistive devices such as a walker.
Important exercises after recovery:
Pull the ball down a second time, then release it. Repeat 10 times. This exercise is crucial for improving blood circulation.
Press your knee down, then pull your glutes towards your hips. This exercise is known as quadriceps curl.
Place a cushion under your knee.
Extend your body with assistance. Repeat 10 times.
Standing exercises:
Alternate between standing on your toes and heels. You can use a weight to counteract gravity.
Stand on one support and try to place your weight on it.
When the knee cartilage is damaged, or there is rheumatoid arthritis, or there is bone involvement, or when the knee cartilage is damaged and unable to support itself, damage occurs in all parts of the knee.
Open-heart surgery: Open-heart surgery is called traditional heart surgery. It is a procedure in which the chest wall is opened to perform surgery on the heart muscle, valves, or arteries. The surgeon makes an incision in the sternum or its upper part. Once the heart is reached, an artificial heart-lung machine is placed to replace the heart and perform its function of pumping blood to all parts of the body. This machine allows the surgeon to operate on a heart that has stopped working and through which blood does not flow. It has become possible to perform this operation through small incisions between the ribs of the rib cage instead of the usual large incision in the sternum. This is called minimally invasive surgery. An artificial heart-lung machine may be used in this type of surgery or omitted. Therefore, the name “open-heart surgery” is sometimes inaccurate. A doctor decides to perform open-heart surgery when other alternatives, such as medication, a healthy lifestyle, and other methods, have been exhausted. The cardiologist assesses the patient’s condition and their need for surgery, conducts the necessary medical tests to determine the patient’s health status, and then discusses the surgery with the patient frankly, explaining its complexity, delicate nature, and potential side effects. The patient then requires a recovery period to begin regaining their health and well-being. Reasons for open-heart surgery include: repairing damaged parts of the heart; replacing or repairing a malfunctioning heart valve; transplanting a healthy heart from a donor to replace the old one; implanting cardiac devices to help control heartbeat and regulate blood flow; and treating heart failure and coronary artery disease. Types of Open Heart Surgery: The following are some types of open heart surgery:
Coronary Artery Bypass Grafting (CABG): This is the most common surgical procedure. It improves blood flow to the heart to treat coronary artery disease, which is caused by the buildup of fatty plaques (cholesterol) inside the coronary arteries. This buildup narrows the arteries, reducing the amount of blood flowing through them and depriving the heart muscle of oxygen. This can cause severe chest pain (angina). If these plaques rupture, they can lead to the formation of large blood clots, which can completely block blood flow through the coronary arteries (heart attack). During this surgery, a healthy artery or vein is connected to the blocked coronary artery to restore blood and oxygen flow to the heart muscle. This procedure can be performed on more than one blocked coronary artery in a single surgery. Repairing or replacing heart valves: For the heart to function properly, blood must flow in only one direction. Heart valves perform this function, opening and closing precisely during the pumping process. When a valve is damaged (severely narrowed, preventing blood flow, or incompletely closed, allowing blood to flow in the opposite direction), open-heart surgery is performed to repair the damaged valve or replace it with a new artificial valve or a biological valve (taken from a cow or human heart). Treatment of atrial fibrillation: This is the most common type of heart rhythm disorder, where the atria contract irregularly or rapidly. A procedure called maze surgery is performed, which involves creating new pathways for electrical signals to travel through the atria to regulate their contractions. Heart transplantation: This procedure involves removing the diseased heart of the patient and replacing it with a healthy heart from a deceased donor. Most heart transplants are performed on patients with heart failure (the end stage of the disease when all other treatments have failed), which is when the heart is too weak or unable to pump enough blood to meet the body’s needs. Implantation of an atrioventricular assist device (VAD): This device is used to support heart function and regulate blood flow in patients with weakened heart muscle or heart failure, or while awaiting a heart transplant. It can be used temporarily for months or years, depending on the patient’s condition. Transcatheter aortic implantation (TAH): This device temporarily replaces the damaged ventricles during heart transplant surgery in cases of chronic heart failure. Medical evaluation and diagnostic tests: The doctor will discuss the following with the patient: the type of heart problem they are experiencing and the symptoms it causes; previous treatments for the patient’s heart problems, including medications or surgeries; family history of heart disease; other health problems the patient has, such as diabetes and high blood pressure; the patient’s age and overall health. Some blood tests may be performed, such as a complete blood count, cholesterol test, and other tests as needed. As for diagnostic tests, they are performed to obtain information about the heart problem and the patient’s overall health. These tests help the doctor decide whether surgery is necessary, determine its type, and estimate the time required. These tests may include: Electrocardiogram (ECG): to determine the electrical activity of the heart (measuring heart rate and rhythm). Stress test: the patient’s heart is examined while they perform exercises prescribed by the doctor. Some heart problems are easier to diagnose when the heart is working harder than normal. Echocardiogram: this test uses ultrasound technology to determine the shape and size of the heart, the condition of its valves, and its electrical activity. Coronary angiography (catheterization)
Intracytoplasmic sperm injection (ICSI) is a sperm-based assisted reproductive technology (ART) used to enhance fertilization in in vitro fertilization (IVF). This involves injecting a single sperm directly into a mature egg, which is then transferred to the woman’s uterus or fallopian tube. ICSI is highly successful, with fertilization occurring in approximately 90% of cases. As with IVF, several factors influence the success of a pregnancy resulting from ICSI. Indications for ICSI: ICSI can be used when there is a reason preventing or hindering fertilization. It is often performed in cases where male infertility is attributed to the man. The situations in which ICSI may be performed include:
Male infertility factors:
These factors include low sperm count, poor sperm motility, poor sperm quality, or the inability of sperm to penetrate the egg. Azoospermia, characterized by the absence of sperm in ejaculate, is another possible cause. There are two types of azoospermia: obstructive and non-obstructive. Obstructive azoospermia occurs due to a vasectomy (cutting the vas deferens), congenital absence of the vas deferens, or scarring from a previous infection. Non-obstructive azoospermia occurs when an abnormal testicle fails to produce sperm. Repeated IVF without success: Intracytoplasmic sperm injection (ICSI) can be used in cases unrelated to sperm problems. For example, some couples choose ICSI after repeated failed IVF attempts. Preimplantation genetic testing (PGT): ICSI is used for couples who plan to test for genetic problems in their embryo. How ICSI works: The ICSI procedure includes the following steps:
Sperm collection: Sperm is collected through masturbation or surgically removed from the testicle through a small incision. Surgery is typically used when there is an obstruction preventing sperm release or a problem with sperm development. If sperm count is low or absent, the doctor may recommend genetic testing to identify any problems. Genetic testing is performed before the start of the IVF process. Ovulation and egg retrieval: The woman is prepared for egg retrieval by taking a combination of medications for two weeks. These medications include gonadotropins or follicle-stimulating hormone (FSH) to stimulate the ovaries to produce multiple eggs. After the first week, estrogen levels are monitored in the blood, and ultrasound is used to check the maturation of the eggs in the follicles. During the second week, the medication dosage may be adjusted based on the test and ultrasound results. If the follicles are fully developed, a dose of human chorionic gonadotropin (hCG) is administered to stimulate follicle maturation. The mature eggs are then retrieved 34 to 36 hours after maturation, either laparoscopically or using an ultrasound-guided needle aspirator inserted through the abdomen into the ovaries. Sperm injection and transfer: The sperm is then fixed The egg is placed in a special glass dish, and a single sperm is added to the same dish to allow fertilization to occur. After fertilization in the laboratory, the fertilized eggs are examined, and one or more are selected for transfer to the uterus using a thin, flexible tube inserted through the cervix. Sometimes, other embryos can be frozen for future use. The disadvantages and risks of in vitro fertilization (IVF) are slightly higher than some other fertility treatments, including: an increased risk of miscarriage due to the use of sperm that may not be able to fertilize the egg; damage to eggs due to the processes involved in the entire procedure; and birth defects. While IVF may affect the embryos born with this procedure, the evidence is not yet conclusive, and more definitive proof is needed. These defects include genetic and physical problems, which have been observed in a small number of cases. A significant number of children born as a result of IVF may have problems such as hypospadias. However, it’s important to note that these defects are often due to the underlying infertility issue, not the treatment itself. There is a possibility of future infertility in the offspring due to inheriting the condition from the male parents. However, doctors emphasize that it’s too early to know for sure, as those conceived through IVF are still teenagers, given the novelty of this infertility treatment. Ovarian hyperstimulation syndrome (OHSS) can be caused by ovulation-stimulating drugs containing hormone therapy, but the risk can be reduced by closely monitoring the ovaries and hormone levels during treatment. Multiple pregnancies are also possible, depending on the number of embryos transferred. Finally, IVF is more expensive than artificial insemination.
Femto-LASIK Procedure
This is a modern LASIK technique that uses a femtosecond laser to separate the corneal layers instead of the traditional mechanical methods used in conventional LASIK. This leads to the following advantages:
The possibility of performing LASIK on thin corneas that are not suitable for conventional LASIK.
The ability to correct refractive errors to a greater degree.
Achieving a cornea with better biomechanical properties.
A faster recovery after LASIK.
Avoiding the problems of older methods, thus increasing the safety of the procedure to an unprecedented level.
Excellent vision quality after LASIK.
Is Femto-LASIK suitable for all cases?
Femto-LASIK is suitable for most cases that are suitable for conventional LASIK. However, it is also suitable for some cases where conventional LASIK is not suitable due to thin corneas or excessive curvature, which can lead to problems with traditional LASIK methods.
The Difference Between LASIK and Femto-LASIK
The LASIK procedure is divided into two main parts. The first part involves preparing the cornea for LASIK by creating a thin flap in the cornea using a precise and sophisticated instrument called a microkeratome. After the flap is created, the LASIK device is used to reshape the cornea and adjust its curvature to correct the measurements.
The Femto-LASIK device performs the preparatory step of creating the corneal flap, which is done by the microkeratome. Therefore, we can tell the patient that the entire procedure, from beginning to end, is laser-assisted. The femtosecond laser is used to create the corneal flap, and the excimer laser is used to reshape the cornea and correct its measurements.
Gastric bypass surgery, also known as gastric bypass, is a weight-loss procedure performed on individuals with obesity. It helps patients lose 60-80% of their excess weight. In most cases, this procedure is performed laparoscopically. Using a laparoscope reduces post-operative pain and speeds up recovery, thus shortening the patient’s hospital stay. After discharge, patients must adhere to the provided instructions to maximize weight loss and minimize the risk of post-operative complications. The gastric bypass surgery typically takes 2-4 hours. The surgeon follows these steps:
The patient is given general anesthesia, so they are asleep during the procedure and feel no pain. The surgeon divides the stomach into two sections, making the upper section smaller and the lower section larger. In reality, after eating, food will be directed to the upper section of the stomach, which can only hold about 28 grams of food or 30 ml of liquid. This forces the person to eat less, thus leading to weight loss, as the goal of this procedure is to reduce the stomach’s size. The surgeon then connects the smaller upper section of the stomach, called the gastric pouch, to a part of the small intestine through a small opening. This allows food to pass from the upper section of the stomach into the small intestine through the created opening. This procedure is called gastric bypass, and its purpose is to reduce the number of calories absorbed by the body. The bypass can be performed either through open surgery or laparoscopically. In open surgery, the surgeon makes a large incision in the abdomen. In laparoscopic surgery, the surgeon uses a small camera inserted into the abdomen to view its interior. The conditions for gastric bypass surgery are that this procedure is not suitable for everyone.
Certain conditions must be met by the applicant:
These include: All previous attempts at weight loss have failed, despite following a healthy diet and exercising regularly. A body mass index (BMI) of 40 or higher is also a possibility. Alternatively, a BMI of 35 or higher, coupled with other weight-related health problems such as high blood pressure, type 2 diabetes, or sleep apnea, is also a possibility. Finally, men must be approximately 45 kg or more overweight, and women approximately 36 kg or more overweight.
Despite its effectiveness in weight loss, gastric bypass surgery can lead to several complications, including: Dumping syndrome: In this condition, food moves too quickly from the stomach into the small intestine. Symptoms after eating include sweating, nausea, diarrhea, fainting, and general weakness. Gastric pouch dilation: The stomach may stretch over time, eventually returning to its original size in many cases. Stomal stenosis: This narrowing of the opening between the upper part of the stomach and the small intestine may cause nausea, acid reflux, vomiting, and difficulty eating, potentially requiring surgery to widen the opening. Gallstones: These can occur as a result of rapid weight loss. Nutritional deficiencies: The body’s ability to absorb nutrients from food decreases, making individuals more susceptible to deficiencies in vitamins, minerals, and other essential nutrients. Staple line rupture or collapse: These staples are used to divide the stomach into two sections in preparation for gastric bypass surgery.
A number of procedures are considered before undergoing this surgery, some of which are listed below: The doctor explains the nature of the procedure the patient will undergo, allowing ample opportunity for questions and inquiries. The patient is asked to sign a medical consent form, giving their approval for the surgery. It is important to read the form carefully and ask questions if anything is unclear. The patient undergoes a complete physical examination to ensure they are in good health, and their complete medical history is reviewed. The patient is also asked to undergo other tests, such as diagnostic or blood tests. A pregnancy test is performed to confirm the absence of pregnancy. It is important to note that pregnancy is not permitted during the first year after the surgery, as rapid weight loss can pose a risk to the life and safety of the fetus. The patient is required to fast for eight hours before the surgery. The doctor must be informed of all aspects of the patient’s health, including any medications or herbal supplements they are taking, any allergies to substances or medications, and any history of bleeding disorders. The patient will be asked to begin exercising and making dietary changes several weeks before surgery.
Can a penile implant be fitted for patients with high blood pressure, diabetes, and heart disease?
Yes, absolutely. The implant is the most suitable option for patients with high blood pressure, diabetes, and heart disease because these patients often experience erectile dysfunction as a result of these conditions. Therefore, it is very safe for them.
How long does penile implant surgery take?
It is a very simple procedure that takes no more than an hour. The patient is discharged from the hospital the same day and can resume normal life within a day or two.
Does the implant treat penile fibrosis?
Penile implant surgery does not treat fibrosis. However, it is known that penile fibrosis can lead to curvature and subsequently erectile dysfunction. The implant corrects the curvature and erectile dysfunction.
Is there only one fixed size for the implant?
No, of course not. There are different sizes available. Penile sizes vary from man to man, and there are techniques during surgery that allow us to determine the appropriate size for each patient based on their penis size, and then fit the implant to the correct size. Can penile implant surgery be performed at any hospital?
Penile implant surgery requires a very high degree of safety, as it involves inserting a foreign object into the body. The body needs to accept the implant within a short period, so the sterilization of the instruments used must be extremely strict. This is why the choice of hospital for the surgery is crucial; it must be a specialized facility, not just any hospital.
When can a man resume sexual activity after the surgery?
A man can resume sexual activity 4 to 6 weeks after the surgery.
Are there different types of penile implants?
Yes, there is a type of penile implant called a “flexible-rigid” or “semi-rigid” implant. It consists of two medical-grade silicone cylinders reinforced internally with silver or nickel. This type provides rigidity during erection, and the penis remains fully erect during intercourse. After intercourse, it can be bent downwards. There is another, newer and more effective type: the hydraulic penile implant. This type is different because it closely mimics a natural erection. The penis remains erect during intercourse, and when not in use, it can be returned to a flaccid state.
There are two types of hydraulic penile implants: a two-piece type, consisting of two hollow silicone cylinders connected to a pump containing saline solution, and a three-piece type, consisting of two hollow silicone cylinders connected to a pump and a separate reservoir for saline solution. This is the newer and more effective type.
What are the disadvantages of using a vacuum device to treat erectile dysfunction?
I am against using vacuum devices to treat erectile dysfunction because this device provides initial results but then becomes a cause of erectile dysfunction itself, as it leads to sagging of the penile tissue.
When can penile implant surgery be repeated?
Penile implant surgery is a permanent procedure performed once in a lifetime, provided it is done correctly. The availability of penile implant surgery, along with the application of modern techniques, has provided a permanent solution to the problem of erectile dysfunction.
The patient is given general anesthesia, so they are asleep during the procedure and feel no pain. The surgeon divides the stomach into two sections, making the upper section smaller and the lower section larger. In reality, after eating, food will be directed to the upper section of the stomach, which can only hold about 28 grams of food or 30 ml of liquid. This forces the person to eat less, thus leading to weight loss, as the goal of this procedure is to reduce the stomach’s size. The surgeon then connects the smaller upper section of the stomach, called the gastric pouch, to a part of the small intestine through a small opening. This allows food to pass from the upper section of the stomach into the small intestine through the created opening. This procedure is called gastric bypass, and its purpose is to reduce the number of calories absorbed by the body. The bypass can be performed either through open surgery or laparoscopically. In open surgery, the surgeon makes a large incision in the abdomen. In laparoscopic surgery, the surgeon uses a small camera inserted into the abdomen to view its interior. The conditions for gastric bypass surgery are that this procedure is not suitable for everyone.
Certain conditions must be met by the applicant:
These include: All previous attempts at weight loss have failed, despite following a healthy diet and exercising regularly. A body mass index (BMI) of 40 or higher is also a possibility. Alternatively, a BMI of 35 or higher, coupled with other weight-related health problems such as high blood pressure, type 2 diabetes, or sleep apnea, is also a possibility. Finally, men must be approximately 45 kg or more overweight, and women approximately 36 kg or more overweight.
Despite its effectiveness in weight loss, gastric bypass surgery can lead to several complications, including: Dumping syndrome: In this condition, food moves too quickly from the stomach into the small intestine. Symptoms after eating include sweating, nausea, diarrhea, fainting, and general weakness. Gastric pouch dilation: The stomach may stretch over time, eventually returning to its original size in many cases. Stomal stenosis: This narrowing of the opening between the upper part of the stomach and the small intestine may cause nausea, acid reflux, vomiting, and difficulty eating, potentially requiring surgery to widen the opening. Gallstones: These can occur as a result of rapid weight loss. Nutritional deficiencies: The body’s ability to absorb nutrients from food decreases, making individuals more susceptible to deficiencies in vitamins, minerals, and other essential nutrients. Staple line rupture or collapse: These staples are used to divide the stomach into two sections in preparation for gastric bypass surgery.
A number of procedures are considered before undergoing this surgery, some of which are listed below: The doctor explains the nature of the procedure the patient will undergo, allowing ample opportunity for questions and inquiries. The patient is asked to sign a medical consent form, giving their approval for the surgery. It is important to read the form carefully and ask questions if anything is unclear. The patient undergoes a complete physical examination to ensure they are in good health, and their complete medical history is reviewed. The patient is also asked to undergo other tests, such as diagnostic or blood tests. A pregnancy test is performed to confirm the absence of pregnancy. It is important to note that pregnancy is not permitted during the first year after the surgery, as rapid weight loss can pose a risk to the life and safety of the fetus. The patient is required to fast for eight hours before the surgery. The doctor must be informed of all aspects of the patient’s health, including any medications or herbal supplements they are taking, any allergies to substances or medications, and any history of bleeding disorders. The patient will be asked to begin exercising and making dietary changes several weeks before surgery.
Can a penile implant be fitted for patients with high blood pressure, A cochlear implant is a surgical procedure that involves implanting an electronic medical device to help deaf people and those with severe hearing loss by directly stimulating the auditory nerve.
How a Cochlear Implant Works
Unlike hearing aids, which amplify sounds, a cochlear implant bypasses the damaged parts of the ear, delivering sound directly to the auditory nerve.
A sound processing device is implanted behind the ear. This device collects sound waves and transmits them to a receiver implanted under the skin behind the ear. The receiver then sends the sound signals to electrodes implanted in the cochlea of the inner ear.
These signals stimulate the auditory nerve, which transmits the signals to the brain, where they are interpreted as audible sounds.
Who is a Candidate for a Cochlear Implant?
Not everyone with hearing problems is a candidate for a cochlear implant. A cochlear implant is the ideal solution in the following cases:
The absence of medical conditions that could increase the risks associated with cochlear implantation.
Those with moderate to severe hearing loss in both ears.
Those who have not benefited from hearing aids. Scoring 50% or less on camel discrimination tests in the ear where the cochlear implant will be placed.
Scoring 60% or less on camel discrimination tests in the ear that will not be implanted, or in both ears with the use of hearing aids.
Cochlear Implant Procedure
After the necessary tests and examinations are conducted, and the patient is deemed a suitable candidate for implantation, the timing of the cochlear implant surgery is determined. The following often occurs during the procedure:
Related Topics
Neck pain and mild gland swelling
Treatment of vaginal yeast infections and hymenal issues
Checking for thyroid nodules
A child with recurrent ear discharge
Administering isotretinoin (Accutane) to a child who cannot swallow capsules
After administering general anesthesia, the surgeon makes an incision behind the ear and a small hole in the cochlea to insert the electrodes. The receiver is then inserted under the skin and secured to the skull, and the incision is closed with sutures.
After the procedure, the patient is transferred to the recovery unit and monitored for any complications. The patient can be discharged from the hospital a few hours after the procedure or the following day.
A follow-up appointment is scheduled approximately one week after the surgery to ensure the wound has healed. A month after the surgery, the external components are fitted, and the implant is then activated. The doctor may make some adjustments in the following months.
To improve hearing, a treatment called auditory rehabilitation is necessary.
Benefits of Cochlear Implantation
Cochlear implantation offers several benefits, including:
Better hearing than hearing aids.
The ability to hear and concentrate even in noisy environments.
The ability to speak on the phone without any problems.
Disadvantages of Cochlear Implantation
Cochlear implantation can cause several disadvantages, such as:
Tinnitus (ringing in the ears).
Vertigo.
Balance problems.
Meningitis.
Facial paralysis.
Loss of any remaining natural hearing.
Removal of the external component when showering or swimming.
Constant battery charging or replacement.
The need for surgery to remove the implant for repair or other reasons.e patient will be asked to begin exercising and making dietary changes several weeks before surgery.
Cochlear Implant
A cochlear implant is a surgical procedure that involves implanting an electronic medical device to help people who are deaf or have severe hearing loss by directly stimulating the auditory nerve.
How a Cochlear Implant Works
Unlike hearing aids that simply amplify sounds, cochlear implants bypass the damaged parts of the ear and deliver sound signals directly to the auditory nerve.
A sound processor is placed behind the ear to capture sound waves and transmit them to a receiver implanted under the skin behind the ear. The receiver then sends signals to electrodes implanted in the cochlea (inner ear). These signals stimulate the auditory nerve, which carries them to the brain where they are interpreted as sound.
Who Is Eligible for a Cochlear Implant?
Not everyone with hearing problems is a candidate. Cochlear implants are most suitable for individuals who:
Do not have medical conditions that increase surgical risks
Have moderate to severe hearing loss in both ears
Do not benefit from hearing aids
Score 50% or less in sentence recognition tests in the ear to be implanted
Score 60% or less in sentence recognition tests in the other ear, or in both ears with hearing aids
Procedure Steps
After necessary tests and confirming eligibility, the surgery is scheduled. Typically:
The procedure is performed under general anesthesia
The surgeon makes an incision behind the ear
A small opening is made in the cochlea to insert the electrodes
The receiver is implanted under the skin and secured to the skull
The incision is then closed with stitches
After surgery, the patient is moved to recovery and monitored for complications. Most patients can leave the hospital within a few hours or the next day.
A follow-up visit is scheduled about a week later to check healing. After about a month, the external components are fitted and the implant is activated. Further adjustments may be made in the following months.
To improve hearing performance, patients should undergo auditory rehabilitation therapy.
Benefits of Cochlear Implants
Better hearing compared to hearing aids
Improved ability to hear and focus in noisy environments
Ability to use the phone more effectively
Risks and Complications
Tinnitus (ringing in the ear)
Dizziness
Balance problems
Meningitis
Facial nerve paralysis
Loss of any remaining natural hearing
Need to remove the external device during bathing or swimming
Regular battery charging or replacement
Possible need for additional surgery to repair or replace the implant
Sleeve gastrectomy, also known as vertical sleeve gastrectomy or tubular sleeve gastrectomy, is the most common weight-loss procedure worldwide.
The procedure involves significantly reducing the size of the stomach by removing a portion of the stomach. It is performed under general anesthesia using advanced laparoscopic surgery.
It is crucial that the procedure be performed by highly experienced surgeons to ensure an asymmetrical final stomach shape.
Otherwise, swallowing difficulties and acid reflux may develop.
Information about Sleeve Gastrectomy
Although the stomach is reduced in size, the procedure does not alter the direction of food flow in the stomach or intestines, nor does it reduce the amount of food that is digested.
This means that all nutrients, including vitamins, minerals, and protein, will continue to be absorbed normally by the body.
It simply reduces the stomach’s capacity from approximately 1.5 liters of food and liquids to about 200 ml.
This allows the person to feel comfortable and full with a meal portion roughly equivalent to a small cup of food. Typically, patients who have undergone gastric sleeve surgery can eat 4-6 small meals a day, which is actually the ideal way to eat.
Nutritionists and obesity and weight loss specialists recommend frequent small meals as a way to avoid large fluctuations in insulin levels and achieve a greater calorie intake as part of a healthy eating pattern.
Despite its reduced size, the stomach lining continues to function normally – food and nutrients continue to enter and exit in the same way, and acid production continues to aid digestion.
How does gastric sleeve surgery treat obesity?
Gastric sleeve surgery works in three different ways:
The significant reduction in stomach size and capacity allows patients to feel full and satisfied after a much smaller meal than they would have eaten before the surgery, thus providing control over food portions.
On another level, the level of the hunger hormone is significantly reduced (individual results may vary), as the portion of the stomach that was removed is rich in cells that produce this hormone.
This makes patients feel consistently less hungry as a result. The procedure alters the way fatty foods are processed by the digestive system. Patients often report a loss of taste for sugary and fatty foods such as chocolate, fried foods, and carbonated drinks, which seem to make them feel bloated and unsettled. This helps patients adopt healthier eating habits.
A corneal transplant can restore vision, reduce pain, and improve the appearance of a damaged or diseased cornea.
Most corneal transplants are successful. However, the procedure carries a small risk of complications, such as rejection of the donor cornea.
Why is it done?
Eye Anatomy
Open pop-up dialog
A corneal transplant is often used to restore vision in someone with a damaged cornea. A corneal transplant may relieve pain or other signs and symptoms associated with corneal diseases.
A number of conditions can be treated with a corneal transplant, including:
A cornea that protrudes outwards (keratoconus)
Fuchs’ dystrophy
Thinning of the cornea
Corneal scarring, caused by infection or injury
Corneal clouding
Corneal swelling
Corneal ulcers, including those caused by infection
Complications from previous eye surgery
Request an appointment at Mayo Clinic
Risks
Corneal transplantation is a relatively safe procedure. However, it carries a small risk of serious complications, such as:
Eye infection
Increased risk of clouding of the eye’s lens (cataracts)
Increased pressure in the eyeball (glaucoma)
Problems with the sutures used to secure the donor cornea
Rejection of the donor cornea
Corneal swelling
Signs and symptoms of corneal rejection
In most cases, the body’s immune system may mistakenly attack the donor cornea. This is called rejection and may require medical treatment or another corneal transplant.
Schedule an appointment with your eye doctor if you notice any signs or symptoms of rejection, such as:
Vision loss
Pain
Redness
Sensitivity to light
Rejection occurs in about 10 percent of corneal transplants.
How to Prepare
Before your corneal transplant surgery, you will undergo the following:
A comprehensive eye exam. Your eye doctor will look for conditions that could cause complications after surgery.
Eye measurements. Your eye doctor will determine the size of the donor cornea you need.
A review of all medications and supplements you take. You may need to stop taking certain medications or supplements before or after your corneal transplant.
Treatment of other eye problems. Eye problems unrelated to surgery, such as infection or inflammation, can reduce the chances of a successful corneal transplant. Your eye doctor will work to resolve these problems before surgery.
Your doctor will discuss what to expect during surgery and explain the risks of the procedure.
Finding a Donor Cornea
Most corneas used in corneal transplants come from deceased donors. Unlike organs such as the liver and kidneys, people who need a corneal transplant won’t have to wait long periods. This is because most people are recommended to donate their corneas after death, unless they have certain conditions, thus making more corneas available for transplantation.
Corneas from donors who had multiple conditions, such as certain central nervous system disorders, infections, eye diseases, previous eye surgeries, or from people who died from unknown causes, may not be used.
What to Expect
During the Procedure
On the day of your corneal transplant, you will be given a sedative to help you relax and a local anesthetic to numb your eye. You will not be asleep during the surgery, but you should not feel any pain.
During the most common type of corneal transplant (penetrating keratoplasty), the surgeon cuts the entire thickness of the abnormal or diseased cornea to remove a small, button-sized disc of corneal tissue. A machine that works like a cookie cutter (a microkeratome) is used to make a precise circular incision.
The donor cornea, cut to fit the patient’s eye, is placed in the opening. The surgeon then uses a thin thread to stitch the new cornea into place. The stitches may be removed at a later visit to your ophthalmologist.
In some cases, if people are not eligible for a donor cornea transplant, doctors may implant an artificial cornea (replacement corneal transplant).
Partial Corneal Transplant Procedures
For some types of corneal problems, a full-thickness corneal transplant is not always the best treatment. Other types of transplants that remove only certain layers of corneal tissue or only the diseased tissue can be used. These procedures include:
Endometrial keratoplasty (EK). This procedure removes diseased tissue from the back layers of the cornea, including the endothelium, along with the posterior endothelial membrane (Décime), a thin layer of tissue that protects the endothelium from injury and infection. Donor tissue is carefully transplanted to replace the removed tissue.
There are two types of endometrial keratoplasty. The most common type, called desmoid keratoplasty (DSEK), uses donor tissue to replace about one-third of the cornea. A newer type of the procedure, called desmoid keratoplasty (DMEK), uses a much thinner layer of donor tissue. Because the tissue used in DMEK is so thin and fragile, it is more complex than DSEK and not as common.
Anterior lamellar keratoplasty (ALK). This procedure removes diseased tissue from the anterior layers of the cornea, including the corneal epithelium and stroma, but leaves the posterior endothelium intact.
The depth of corneal damage determines which type of ALK procedure is right for you. Superficial anterior lamellar keratoplasty (SALK) replaces only the anterior layers of the cornea, leaving the healthy corneal epithelium intact. Deep anterior lamellar keratoplasty (DALK) is used when the corneal damage extends deeper into the occlusion.
How a Cochlear Implant Works
Unlike hearing aids, which amplify sounds, a cochlear implant bypasses the damaged parts of the ear, delivering sound directly to the auditory nerve.
A sound processing device is implanted behind the ear. This device collects sound waves and transmits them to a receiver implanted under the skin behind the ear. The receiver then sends the sound signals to electrodes implanted in the cochlea of the inner ear.
These signals stimulate the auditory nerve, which transmits the signals to the brain, where they are interpreted as audible sounds.
Who is a Candidate for a Cochlear Implant?
Not everyone with hearing problems is a candidate for a cochlear implant. A cochlear implant is the ideal solution in the following cases:
The absence of medical conditions that could increase the risks associated with cochlear implantation.
Those with moderate to severe hearing loss in both ears.
Those who have not benefited from hearing aids. Scoring 50% or less on camel discrimination tests in the ear where the cochlear implant will be placed.
Scoring 60% or less on camel discrimination tests in the ear that will not be implanted, or in both ears with the use of hearing aids.
Cochlear Implant Procedure
After the necessary tests and examinations are conducted, and the patient is deemed a suitable candidate for implantation, the timing of the cochlear implant surgery is determined. The following often occurs during the procedure:
Related Topics
Neck pain and mild gland swelling
Treatment of vaginal yeast infections and hymenal issues
Checking for thyroid nodules
A child with recurrent ear discharge
Administering isotretinoin (Accutane) to a child who cannot swallow capsules
After administering general anesthesia, the surgeon makes an incision behind the ear and a small hole in the cochlea to insert the electrodes. The receiver is then inserted under the skin and secured to the skull, and the incision is closed with sutures.
After the procedure, the patient is transferred to the recovery unit and monitored for any complications. The patient can be discharged from the hospital a few hours after the procedure or the following day.
A follow-up appointment is scheduled approximately one week after the surgery to ensure the wound has healed. A month after the surgery, the external components are fitted, and the implant is then activated. The doctor may make some adjustments in the following months.
To improve hearing, a treatment called auditory rehabilitation is necessary.
Benefits of Cochlear Implantation
Cochlear implantation offers several benefits, including:
Better hearing than hearing aids.
The ability to hear and concentrate even in noisy environments.
The ability to speak on the phone without any problems.
Disadvantages of Cochlear Implantation
Cochlear implantation can cause several disadvantages, such as:
Tinnitus (ringing in the ears).
Vertigo.
Balance problems.
Meningitis.
Facial paralysis.
Loss of any remaining natural hearing.
Removal of the external component when showering or swimming.
Constant battery charging or replacement.
The need for surgery to remove the implant for repair or other reasons.e patient will be asked to begin exercising and making dietary changes several weeks before surgery.
What is bladder cancer?
Bladder cancer is cancer that originates in the lining of the bladder. The bladder is a hollow organ in the lower abdomen that stores urine before it is released from the body. This type of cancer most often affects adults.
What causes bladder cancer?
The exact causes of bladder cancer are unknown, but several risk factors have been identified that can increase the chance of developing it. Men are three times more likely to develop the disease than women, and middle-aged people (over 50) and older adults are more likely to develop bladder cancer than younger people. There is also a link between bladder cancer and several preventable environmental factors, such as:
Smoking: Smokers are twice as likely to develop bladder cancer as non-smokers.
Exposure to chemicals: Some chemicals used in industries such as dyes, paints, and textiles are at increased risk.
People with chronic bladder infections, such as recurrent bladder infections and other urinary tract problems, are at increased risk.
What are the symptoms of bladder cancer?
Blood in the urine is the most common symptom. Other symptoms include a burning or painful sensation when urinating and frequent urination.
How is bladder cancer diagnosed?
Tests used to diagnose bladder cancer include:
Urinalysis: to look for any abnormalities in the urine. Urine cytology: a specialized test to examine the cells lining the bladder (those excreted in the urine) under a microscope to look for any cancerous cells.
Cystoscopy: a thin tube with a camera at its end is inserted into the bladder to examine the bladder lining.
Bladder biopsy.
CT scan of the abdomen and pelvis.
Other tests to check for tumor spread, such as bone scans, chest X-rays, and CT scans.
How is bladder cancer treated?
For superficial bladder cancer, after an initial diagnostic cystoscopy, all patients undergo transurethral resection of the bladder (TURR). In many cases, the tumor is completely removed, and in these instances, TURR can be considered a definitive cure. However, it is sometimes advisable to administer additional treatment called adjuvant therapy, which involves drugs administered directly into the bladder and is known as intravesical therapy.
The type of adjuvant therapy used depends on the individual risk of recurrence or tumor progression, as well as the patient’s tolerance to the side effects of the treatment.
A further transurethral resection of bladder cancer is recommended for some selected patients with high-risk tumors, either before or after intravesical therapy, to detect any residual disease and to provide a more accurate stage of the disease.
Muscular Bladder Cancer
Standard treatment for muscular bladder cancer includes:
Radical cystectomy. In male patients, this involves the complete removal of the bladder and all visible tissue from the tumor, as well as the urethra, prostate, seminal vesicles, lower ureters, and pelvic lymph nodes. In female patients, radical cystectomy involves the removal of the bladder, all visible and resectable tumors, the entire urethra, the lower part of the ureter, the adjacent portion of the vagina, the uterus, and the pelvic lymph nodes.
These procedures may be slightly modified in some patients to preserve certain organs. This depends on the extent of the tumor, and therefore requires a careful individual assessment.
Radical cystectomy may result in the loss of bladder function, which is the storage of urine. In such cases, the surgeon will connect the ureter to a new outlet to allow urine to drain. This is called urinary diversion. The new outlet may be the urethra, the abdominal wall, or the lower part of the large intestine. The choice of method depends on several factors, including the stage of the disease, the patient’s overall health, and the patient’s preference.
The purpose of kidney stone fragmentation
Kidney stone fragmentation is used to treat kidney stones that are:
larger than 2 centimeters in diameter.
large in size, formed due to infection (hard stones/calculi).
obstructing the flow of urine out of the kidney.
cannot be broken up by extracorporeal shock wave lithotripsy (ESWL).
Procedure
During kidney stone fragmentation, the surgeon makes a small incision in the back to remove the stone from the kidney. A hollow tube is then inserted into the kidney, and a detector is passed through this tube. During percutaneous lithotripsy, the doctor extracts the stone through the tube (breaking and fragmenting the kidney stone through the skin, and then removing the fragments through the tube).
Kidney stone fragmentation is performed under general anesthesia, sometimes under local anesthesia, or even spinal anesthesia. During the procedure, and until complete recovery, urine is drained from the patient’s kidney through a small tube (catheter).
Kidney stone fragmentation is considered a 95% successful procedure, with a success rate of approximately 88% for stones located in the urethra.
Risks of Kidney Stone Fragmentation
Bleeding
Kidney perforation – these perforations generally heal without the need for additional external treatment.
Injury to other internal organs such as the bladder or intestines.
Impairment of normal kidney function.
Despite its importance and effectiveness, kidney stone fragmentation procedures are technically complex.
In addition, it may be necessary to push the removed stone back towards the kidney using a small instrument called a urethroscope so that the surgeon can actually remove it from the system.
Kidney stone fragmentation procedures are performed more frequently using this method than extracorporeal shock wave lithotripsy (ESWL). However, all stone fragments must be removed to prevent them from growing back and forming new stones.
In mastectomy, when very delicate tissue covers the rib cage, complications are frequent (infections, exposure of the implant to external factors), often resulting in subpar outcomes. To overcome this obstacle, we developed a fat grafting technique known as “filling,” performed before reconstruction to increase the thickness of the tissue covering the implant. This method significantly improves the quality of results and reduces complications, allowing for breast reconstruction with implants in a larger number of patients and thus reducing the need for incisions.
Fat is extracted via liposuction (from the abdomen, hips, or thighs) and then injected under the chest skin before implant placement. Two filler procedures are often required to achieve a satisfactory result.
Types of Breast Implants: The silicone gel-filled implant is the most commonly used because it leads to better results. However, a few years ago, this type of implant raised concerns among international medical authorities. Since then, however, several scientific studies have confirmed its reliability and safety. For more information
There are two types of breast implants:
A body-contouring implant, which can be customized in width, length, and projection.
For breast reconstruction, we primarily use a body-contouring implant filled with silicone gel. To augment the other breast, when necessary, we use a rounded implant.
An expandable implant allows the tissues to gradually stretch. It is placed in the appropriate position in a vacuum, and once the skin and muscle have healed, the surgeon injects it with serum through a valve under the skin to increase its volume.
The surgical procedure:
The surgeon makes an incision along the contour of the mastectomy scar.
The surgeon creates a cavity behind the pectoral muscle (the space for implant placement).
The surgeon creates a groove under the breast (the inframammary fold).
The implant is implanted alongside a drainage pad, which will be removed after a few days.
The skin wall is closed.
If necessary, surgery is performed on the opposite breast. Depending on the condition of the breast, it can be augmented (with implants), reduced in size, or its sagging corrected by breast reconstruction.
Procedure
The surgery takes between 1 hour and 30 minutes and 2 hours and 30 minutes.
General anesthesia is administered.
Hospitalization lasts from 24 hours (overnight) to one week, depending on the patient’s location.
Pain is usually mild and can be effectively managed with analgesics.
Dresses are worn for 8 to 10 days.
Sports activities should be avoided for approximately one month.
This surgery is covered by health insurance.
Potential Complications
Introducing a foreign object carries a risk of infection, which can be exacerbated by radiation therapy.
The scar tissue presents a weak point. Radiation therapy also increases the risk of scar tissue failure. The implantation of a replacement organ results in the formation of a capsule, a type of membrane or scar tissue that isolates the organ from surrounding tissues. The quality of the reconstruction depends on the capsule’s flexibility. The more rigid the capsule (forming a scab), the more difficult the reconstruction will be. Furthermore, parietal radiation therapy increases the risk of scab formation.
Testicular prosthesis implantation is used when a patient has lost one or both testicles due to removal, accidental injury, or other reasons. In such cases, an artificial testicle can be implanted to restore the natural appearance of the scrotum. The artificial testicle has the same weight, shape, and feel as a natural testicle and is available in various sizes to ensure a good fit for the patient’s body. The artificial testicle is used solely to improve appearance and alleviate psychological concerns. It does not have any of the functions of a real testicle. Artificial testicles have been used since the 1940s and were previously made from a variety of materials. Nowadays, they are primarily made of silicone rubber and are filled with either silicone gel or saline solution.
What are the conditions that warrant testicular prosthesis implantation? Testicular prosthesis is used in cases of malformation or absence at birth; surgical removal due to injury, such as severe testicular torsion; undescended testicles; removal due to infection; removal for testicular cancer treatment; and female-to-male gender reassignment surgery.
What are the characteristics of a good artificial testicle?
An ideal artificial testicle should:
Have no chemical reaction with the body; not cause infections; be resistant to mechanical stress from movement; be well-sterile; be able to withstand the testicle and maintain the correct shape; and provide comfort to the patient.
How is testicular prosthesis implantation performed?
For testicular prosthesis implantation surgery, a silicone prosthesis filled with saline solution is used. It is fully FDA-approved and does not react with body tissues or cause any complications. The standard surgical procedure is as follows:
The surgery is performed in a state-of-the-art hospital and requires only a short hospital stay. The patient is placed under either general (full body) anesthesia or local anesthesia, which will numb the lower body.
A small incision is typically made in the scrotum.
The artificial testicle is then implanted.
The artificial testicle is secured in place so that it is in the correct position and remains stable.
The incision is closed with cosmetic sutures that leave no visible scar after the wound heals.
As you can see, the artificial testicle implantation is a simple, same-day surgical procedure that takes 30-60 minutes under anesthesia. The artificial testicle is placed in its correct position within the scrotum through a small incision. It is then saturated with an antibiotic solution and examined to ensure proper placement. The incision is then closed with multiple layers of cosmetic sutures that leave no visible scar. The patient returns home the same day and needs to rest for three days before resuming normal activities, while avoiding strenuous activity and sexual activity. Sexual intercourse is possible three to four weeks after the procedure.
What to expect after testicular prosthesis surgery?
Some pain and discomfort in the surgical area can be expected for at least 24 to 48 hours. This pain can be managed with pain medication.
The dressings will remain in place for at least a few days.
The ability to urinate is not affected.
Wearing supportive underwear is recommended.
Heavy lifting, cycling, and strenuous physical activity should be avoided for about a month after surgery.
Fat is extracted via liposuction (from the abdomen, hips, or thighs) and then injected under the chest skin before implant placement. Two filler procedures are often required to achieve a satisfactory result.
Types of Breast Implants: The silicone gel-filled implant is the most commonly used because it leads to better results. However, a few years ago, this type of implant raised concerns among international medical authorities. Since then, however, several scientific studies have confirmed its reliability and safety. For more information
There are two types of breast implants:
A body-contouring implant, which can be customized in width, length, and projection.
For breast reconstruction, we primarily use a body-contouring implant filled with silicone gel. To augment the other breast, when necessary, we use a rounded implant.
An expandable implant allows the tissues to gradually stretch. It is placed in the appropriate position in a vacuum, and once the skin and muscle have healed, the surgeon injects it with serum through a valve under the skin to increase its volume.
The surgical procedure:
The surgeon makes an incision along the contour of the mastectomy scar.
The surgeon creates a cavity behind the pectoral muscle (the space for implant placement).
The surgeon creates a groove under the breast (the inframammary fold).
The implant is implanted alongside a drainage pad, which will be removed after a few days.
The skin wall is closed.
If necessary, surgery is performed on the opposite breast. Depending on the condition of the breast, it can be augmented (with implants), reduced in size, or its sagging corrected by breast reconstruction.
Procedure
The surgery takes between 1 hour and 30 minutes and 2 hours and 30 minutes.
General anesthesia is administered.
Hospitalization lasts from 24 hours (overnight) to one week, depending on the patient’s location.
Pain is usually mild and can be effectively managed with analgesics.
Dresses are worn for 8 to 10 days.
Sports activities should be avoided for approximately one month.
This surgery is covered by health insurance.
Potential Complications
Introducing a foreign object carries a risk of infection, which can be exacerbated by radiation therapy.
The scar tissue presents a weak point. Radiation therapy also increases the risk of scar tissue failure. The implantation of a replacement organ results in the formation of a capsule, a type of membrane or scar tissue that isolates the organ from surrounding tissues. The quality of the reconstruction depends on the capsule’s flexibility. The more rigid the capsule (forming a scab), the more difficult the reconstruction will be. Furthermore, parietal radiation therapy increases the risk of scab formation.
Types of Vaginal Rejuvenation Surgery
Vaginoplasty, or cosmetic vaginal surgery, is a cosmetic and reconstructive surgery of the vaginal canal and its mucous membranes or structure, which may be deformed due to a congenital defect or acquired causes during life such as cancer or trauma. There are several types of this surgery, each with its own indications and different techniques. The most common are:
Vaginal Tightening
Vaginal Lift (or Vaginal Prolapse Correction)
Labial Reshaping
Labial Augmentation or Reduction
Labiaplasty
Labiaplasty is a cosmetic surgery that aims to alter the labia minora (inner labia) or labia majora (outer labia). Excess clitoral hood can also be removed.
In fact, the size, color, and shape of the labia vary considerably from woman to woman, and these labia can also change as a result of childbirth, aging, and other events. There are certain requirements for labiaplasty: being over 18 years of age, in good physical health, and having a healthy body mass index (BMI).
There are various reasons for undergoing labiaplasty, including dissatisfaction with the size and shape of the labia minora or large labia, pain during intercourse, hygiene issues, and urinary tract infections.
A 2008 survey indicated that 32% of women who underwent the procedure did so to correct a “functional” issue, while 31% did so for both functional and cosmetic reasons. The study also found that 37% of women underwent the procedure solely for cosmetic reasons. According to another study conducted in 2011, between 90% and 95% were satisfied with the results. However, there are some risks associated with this cosmetic procedure, including permanent scarring, infection, bleeding, irritation, and even nerve damage, which can lead to increased or decreased sensitivity in the area.
Anatomical images of the vulva are rarely seen in popular media or advertisements, and are even seldom included in anatomy textbooks. Furthermore, most societies oppose sex education. All of this has contributed to a lack of information about natural variations in the labia. Consequently, many women have limited knowledge of vulvar anatomy and its components and are unable to distinguish between what is “normal” and what is “altered.” At the same time, numerous pornographic images circulating online depict the female genitalia in a completely different way, but these are in fact digitally manipulated images where the size and shape of the labia are altered to conform to censorship standards in various countries. Medical researchers have raised concerns about the prevalence of online pornography, which may lead some women to become dissatisfied with their bodies, prompting them to undergo cosmetic surgery and other procedures.
Labial Size
The size of the labia varies from woman to woman. In some cases, the labia minora remain hidden beneath the labia majora, while in others, the labia minora are clearly visible, especially when standing.
From a scientific and medical perspective, there is no fixed normal size for the labia minora. In fact, the size of the labia minora varies from person to person. The color and size of the labia minora in women depend on age, genetics, hormones, and pregnancy.
The size, shape, and color of the labia minora can change significantly throughout life. Usually, one labia is larger than the other. The labia minora may be covered by the labia majora or protrude from them. The labia minora may become larger with sexual arousal; sometimes doubling or tripling their normal diameter. The size of the labia minora may also change after childbirth.
Are there any specific diseases or health conditions that would prevent labiaplasty?
Doctors may advise against such cosmetic procedures in some cases for several reasons, including:
When the labia minora are very small, making it difficult to alter them.
If the woman has an infectious disease or a tumor.
Women who smoke, especially those unwilling to quit, either temporarily or permanently.
Women who experience difficulty in wound healing.
Women who undergo such procedures solely for cosmetic purposes. (Rare cases)
The procedure should not be performed during menstruation to minimize hormonal effects and reduce the risk of infection.
How is labiaplasty performed?
Labisplasty can be performed under local, general, or procedural anesthesia. Before the incision, an anesthetic solution (lidocaine + epinephrine in saline) is injected into the labia minora to induce swelling and constrict blood flow, thus reducing bleeding.
Types of labiaplasty
Edge resection technique
The edge resection technique is the primary technique for labiaplasty and involves a simple cut from the free edge to the small edge. In one incision method, a clip is placed around the vulvar edges, cutting off blood flow to prevent bleeding. After the incision, the labia minora or majora are sutured. Many surgeons prefer this method for its ease of use. A disadvantage is that it removes the natural creases of the free edges of the labia minora, resulting in an unnatural appearance of the vulva. Additionally, this method carries a high risk of nerve damage. Another drawback is the inability to remove excess clitoral skin. Furthermore, the procedure may result in clitoral deformities, necessitating further corrective surgery. One advantage of this method is the removal of dark, irregular vulvar edges through a linear incision.
Central Wedge Resection Technique
The central wedge resection technique involves cutting and removing tissue.
What are the conditions that warrant testicular prosthesis implantation? Testicular prosthesis is used in cases of malformation or absence at birth; surgical removal due to injury, such as severe testicular torsion; undescended testicles; removal due to infection; removal for testicular cancer treatment; and female-to-male gender reassignment surgery.
What are the characteristics of a good artificial testicle?
An ideal artificial testicle should:
Have no chemical reaction with the body; not cause infections; be resistant to mechanical stress from movement; be well-sterile; be able to withstand the testicle and maintain the correct shape; and provide comfort to the patient.
How is testicular prosthesis implantation performed?
For testicular prosthesis implantation surgery, a silicone prosthesis filled with saline solution is used. It is fully FDA-approved and does not react with body tissues or cause any complications. The standard surgical procedure is as follows:
The surgery is performed in a state-of-the-art hospital and requires only a short hospital stay. The patient is placed under either general (full body) anesthesia or local anesthesia, which will numb the lower body.
A small incision is typically made in the scrotum.
The artificial testicle is then implanted.
The artificial testicle is secured in place so that it is in the correct position and remains stable.
The incision is closed with cosmetic sutures that leave no visible scar after the wound heals.
As you can see, the artificial testicle implantation is a simple, same-day surgical procedure that takes 30-60 minutes under anesthesia. The artificial testicle is placed in its correct position within the scrotum through a small incision. It is then saturated with an antibiotic solution and examined to ensure proper placement. The incision is then closed with multiple layers of cosmetic sutures that leave no visible scar. The patient returns home the same day and needs to rest for three days before resuming normal activities, while avoiding strenuous activity and sexual activity. Sexual intercourse is possible three to four weeks after the procedure.
What to expect after testicular prosthesis surgery?
Some pain and discomfort in the surgical area can be expected for at least 24 to 48 hours. This pain can be managed with pain medication.
The dressings will remain in place for at least a few days.
The ability to urinate is not affected.
Wearing supportive underwear is recommended.
Heavy lifting, cycling, and strenuous physical activity should be avoided for about a month after surgery.
Fat is extracted via liposuction (from the abdomen, hips, or thighs) and then injected under the chest skin before implant placement. Two filler procedures are often required to achieve a satisfactory result.
Types of Breast Implants: The silicone gel-filled implant is the most commonly used because it leads to better results. However, a few years ago, this type of implant raised concerns among international medical authorities. Since then, however, several scientific studies have confirmed its reliability and safety. For more information
There are two types of breast implants:
A body-contouring implant, which can be customized in width, length, and projection.
For breast reconstruction, we primarily use a body-contouring implant filled with silicone gel. To augment the other breast, when necessary, we use a rounded implant.
An expandable implant allows the tissues to gradually stretch. It is placed in the appropriate position in a vacuum, and once the skin and muscle have healed, the surgeon injects it with serum through a valve under the skin to increase its volume.
The surgical procedure:
The surgeon makes an incision along the contour of the mastectomy scar.
The surgeon creates a cavity behind the pectoral muscle (the space for implant placement).
The surgeon creates a groove under the breast (the inframammary fold).
The implant is implanted alongside a drainage pad, which will be removed after a few days.
The skin wall is closed.
If necessary, surgery is performed on the opposite breast. Depending on the condition of the breast, it can be augmented (with implants), reduced in size, or its sagging corrected by breast reconstruction.
Procedure
The surgery takes between 1 hour and 30 minutes and 2 hours and 30 minutes.
General anesthesia is administered.
Hospitalization lasts from 24 hours (overnight) to one week, depending on the patient’s location.
Pain is usually mild and can be effectively managed with analgesics.
Dresses are worn for 8 to 10 days.
Sports activities should be avoided for approximately one month.
This surgery is covered by health insurance.
Potential Complications
Introducing a foreign object carries a risk of infection, which can be exacerbated by radiation therapy.
The scar tissue presents a weak point. Radiation therapy also increases the risk of scar tissue failure. The implantation of a replacement organ results in the formation of a capsule, a type of membrane or scar tissue that isolates the organ from surrounding tissues. The quality of the reconstruction depends on the capsule’s flexibility. The more rigid the capsule (forming a scab), the more difficult the reconstruction will be. Furthermore, parietal radiation therapy increases the risk of scab formation.
Travecare Health Tourism Network
is dedicated to delivering exceptional healthcare and tourism services in Egypt. Through our integrated medical complex and an extensive network of top-tier hospitals and specialized centers, we ensure world-class medical care at competitive prices across a wide range of specialties.
We continuously expand our medical partnerships to include only the most trusted and certified providers who meet international quality standards.